Common Spinal Conditions
Posted by Phil Heler on January 18, 2016Common back problems include spondylolisthesis, ankylosing spondylitis, Scheuermann's kyphosis, and osteoporosis.
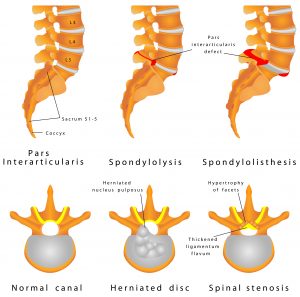
Spondylolisthesis
Typical symptoms: Although this condition can be stable it can also cause general lower back combined with buttock pain. In rare advanced cases it can cause spinal cord or nerve root compression.
Spondylolisthesis is a common back problem in which a vertebra (typically in the lower back) in your back slides forward over the vertebra below it. This may be caused by:
- A defective joint that you’ve had since birth (congenital)
- A joint damaged by an accident or other trauma
- A vertebra with a stress fracture caused from overuse of the joint (e.g. gymnastics or weightlifting)
- A joint damaged by an infection or arthritis.
Sometimes you may be lucky enough to not have any symptoms at all or none until years later. However, it can cause general lower back pain or buttock pain.
In more extreme, cases however, it can cause the spinal cord or nerve roots to be compressed. This can cause back pain and numbness or weakness in one or both legs. In rare cases, it can also impinge or your bladder or bowel control. It is essential that you see a doctor right away if you begin losing bladder or bowel control.
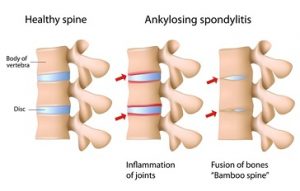
Ankylosing Spondylitis
Typical symptoms: Occurs typically in young adults with slow progressive stiffening of the spine combined with buttock and hip pain.
This is an inflammatory condition of the back that generally affects young adults. It typically begins with inflammation of the sacroiliac joints and generally causes pain and stiffness in both your buttocks and lower back. It follows a typical pattern and is usually worse in the morning but tends to improve with exercise.
People usually feel very fatigued and there can be pain in other parts of the body such as the hips. The condition will lead to a slow progressive stiffening of the spine.
Key to management is early diagnosis so that a regime of preventative exercises can help counteract the general stiffness. Blood tests and X rays can help establish a diagnosis.
Typical characteristics overall include the following:
- Starts before the age of 40 years
- Has been present for at least 3 months
- Has come on slowly over time
- Is worse in the mornings
- Causes stiffness in the mornings lasting for at least 30 minutes (stiffness is perhaps best described as the sort of aching you get the day after heavy exercise)
- Improves with exercise, and is worse with rest
- Improves with anti-inflammatory drugs (e.g. ibuprofen)
- Can wake people from sleep, often in the second half of the night
- Can often cause pain in the buttocks, but rarely pain shooting down the leg (sciatica).
We can offer advice on treatment and recommend an appropriate course of action.
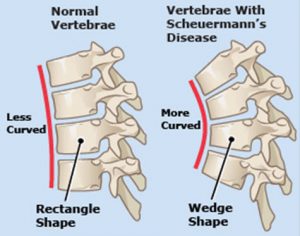
Scheuermann’s Kyphosis
Typical symptoms: Young adults with an emphasised curve in their mid-back combined with spinal pains.
This condition (also known as Scheuermann’s disease) occurs when the front of a vertebral body does not grow as fast and develop as quickly as the back of the vertebra. The vertebrae therefore become wedge-shaped, with the narrow part of the wedge at the front of the spine nearest your tummy.
The wedge-shape of the vertebra creates an increase in the amount of normal curvature in the spine in the mid-back region. This is called a kyphosis and a small amount of curvature is normal but with this condition the curvature can become excessive.
Treatment of Scheuermann’s kyphosis will mainly comprise pain relief and if required the correction of an unacceptable cosmetic deformity. This will prevent potential progression or worsening of the curve.
Treatment will vary depending on the severity of the curve, the flexibility of the curve, the patient’s age and the patient’s preferences. Bracing or casting may be used to attempt to halt the curve’s progression or alternatively ensuing surgery may be necessary.
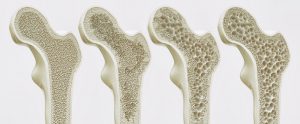
Osteoporosis
Typical symptoms: Spinal pain, occurs with age and has a greater incidence rate in ladies who experience early menopause.
Osteoporosis is characterised by loss of bone density, as most of us already know. This is defined by the World Health Organisation as bone density more than 2.5 standard deviations (SD) below average. Values between 1-2.5 SD below average are termed osteopenic. Bone density decreases with age. In men this occurs slowly, reaching a fracture level risk in the seventies and eighties. However, for some women there can be an accelerated loss in bone density in the ten years after menopause, leading to a significant risk of fracture.
Risk factors include alcohol consumption, smoking, family history, lack of exercise, obviously both age and early menopause. Pain from osteoporosis often occurs because of small fractures in vertebra causing corresponding spinal pain.
There are often initially very few obvious physical signs of osteoporosis. If it is thought that you may have osteoporosis, however, it may be suggested that you have a DEXA (dual energy x-ray absorptiometry) scan to measure the density of your bones and assess your risk of fractures. The scan is available at many hospitals and involves lying on a couch, fully clothed, for about 15 minutes while your bones are x-rayed.
Normal – Your risk of a low-impact fracture is low.
Osteopenia – Your bone is becoming weaker, but your risk of a low-impact fracture is still quite small. You may not need treatment, but you should discuss with your doctor how you can reduce your risk factors.
Osteoporosis – You have a greater risk of low-impact fractures and it’s likely that you’ll need treatment.