Cervical Cancer is Now a Rare Disease Thanks to our National Vaccination Programme
Posted by Phil Heler on November 14, 2021One of the greatest scientific achievements at the beginning of the 21st century was the development of the cervical cancer vaccine. The effects of the UK national vaccination programme for cervical cancer, introduced in 2008, have just been published in the scientific journal ‘The Lancet’.
In 1784 Robert Burns composed the poem ‘Man was Made to Mourn’. This melancholic poem contains the immortal line ‘man’s inhumanity to man’. This phrase has been displayed throughout history with two key examples being the slave trade to the Americas and Caribbean and the holocaust in World War Two. Key historical figures with racist legacies have recently raised controversy.
The 5.5 metre statue of Edward Colston was famously toppled in Bristol in 2020. In 1690 Edward Colston joined the Royal African Company (RAC) that had a monopoly on the West African slave trade. The RAC is estimated to have sold about 100,000 West African people in the Caribbean and the Americas between 1672 and 1689. Colston was a member of the governing body of RAC.
He eventually went on to become a well-known philanthropist making generous donations to various local causes. Besides his statue, there are many places in Bristol that bear his name. There is Colston’s, an independent school; a concert hall, Colston Hall; a high-rise office block, Colston Tower; Colston Street and Colston Avenue. In the context of today however it is understandably argued that ‘he does not represent a diverse and multicultural city’. But just how far do we go in re-writing history?
One scientific pioneer currently under scrutiny is Johannes Stark who won the Nobel Prize for Physics in 1919. His discovery, that became known as the ‘Stark Effect’, about how electric fields influence atoms, was one of the great early discoveries of quantum mechanics.
However, unfortunately he progressed to become a key member of the Nazi scientific establishment and he took an active role in persecuting Jewish scientists. So, in this case the question remains – is the naming of a scientific concept different from bestowing an honour such as a statue? This week I am writing about a less contentious Nobel Prize winner whose discoveries led to an almost complete eradication of cervical cancer.
Vaccines are a miracle of modern science and medicine. They are incredibly important for public health, as we are now only too aware in a time of pandemic. They have saved millions of lives and have eradicated many infectious diseases.
Throughout the twentieth century, great and famous achievements were made with vaccines for diphtheria, measles, mumps, rubella, polio, smallpox and cholera vaccines to name but a few.
One of the greatest scientific achievements at the beginning of the 21st century was the development of the cervical cancer vaccine. The effects of the UK national vaccination programme for cervical cancer, introduced in 2008, have just been published on November 3rd, 2021, in the scientific journal ‘The Lancet’. This study neatly demonstrates the power of science.
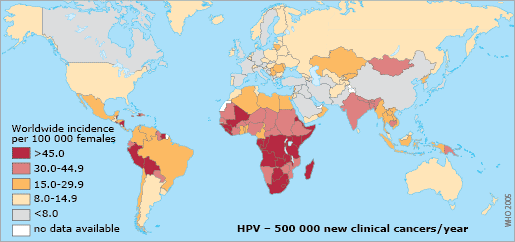
In 2018 there were an estimated 570,000 global cases of cervical cancer and 311,000 deaths from the disease. Globally it was the third most common female cancer after breast (1.38 million cases) and colorectal cancer (0.57 million).
In 2021 in the UK, it is now not even ranked in the 20 most common cancers, and it now accounts for just 1% of all cancers. We, in the UK, are lucky because, of the 311,000 deaths that occur globally from this disease, 85% of these mortalities are in low- and middle-income countries. Often in these countries there is limited access to preventative measures, and it is often not identified until it has progressed, and symptoms develop.
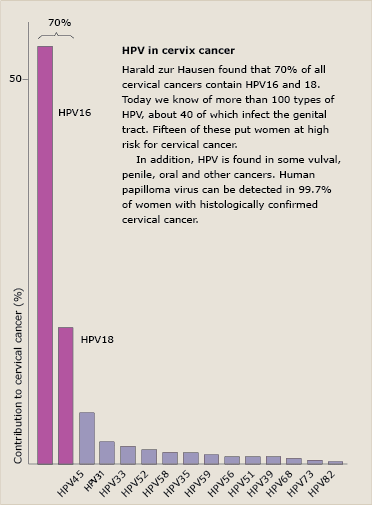
Cervical cancer, more than the other major cancers, typically affects women less than 45 years old. It is caused by the human papillomavirus (or HPV). Human papillomavirus is the most common viral infection of the reproductive tract. There are over 100 types of HPV, and many do not cause any problems but at least 40 of these infect the human genital tract. A few can develop into diseases such as genital warts (HPV 6 and 11) or cancer (HPV16 and 18).
HPV infections usually clear up without any intervention within a few months of acquisition, and about 90% clear within 2 years. A small proportion of infections with certain types of HPV can persist and progress to cervical cancer. There are currently 14 known high risk HPV viruses, two of which, HPV16 and HPV18, are responsible for most HPV-related cancers. Thankfully we have the means to protect against these high-risk viral types by way of the HPV vaccines. But who do we have to thank for this discovery?
The answer to this question is a German virologist called Harald zur Hausen. He was jointly awarded the Nobel Prize for Physiology and Medicine in 2008 for his efforts. He fully deserved his prize, because his theories that were originally conceived in the 1970’s were very much against the prevailing views of the day.
He had isolated HPV strains in cervical cancer tumours, and he strongly suspected that HPV was a causal agent. He assumed that the HPV viral DNA was integrated into the genome of the tumour cells. This is a theory that he eventually proved to be correct.
Following Harald zur Hausen’s work, it was discovered that HPV caused other cancers including anal, vulval, and oral. Disappointingly Harald zur Hausen suggested the idea of an HPV vaccine in 1986, but his idea was not supported by pharmaceutical companies.
The HPV vaccine was eventually developed by the University of Queensland Professors Ian Frazer and Jian Zhou. Their vaccine was based on developing what is known as ‘virus-like particles’ (or VLPs). These VLPs contain protein fragments from the outer coat of the HPV virus, and they are not infectious because they do not comprise any of the virus’s DNA.
However, they do have the benefit of closely resembling the natural virus. Antibodies that are made by our bodies to counteract VLPs are also strongly immunogenic against HPV. This method of vaccination using VLPs is highly effective, as the VLPs cause high levels of antibody production.
Frazer and Zhou’s findings were first presented to the scientific community in 1991. But vaccine design and subsequent trials can take a long time. In fact, it took another 15 years. This might heighten our appreciation for COVID-19 vaccine development in 2020.
It was not until 2006 therefore, following extensive clinical trials that proved the vaccine gave almost 100% protection against HPV 16 and 18, that the vaccine (called Gardasil) was approved for use by Australia and the USA. By 2007 the vaccine was approved in 80 countries. Since then, two further vaccines have been approved called Cervarix (approved in 2007 ) that also prevents HPV16 and 18 and Gardasil 9 in 2014 that protects against nine HPV types (HPV 6, 11, 16, 18, 31, 33, 45, 52, and 58).
As of October 2019, 100 countries worldwide vaccinate against HPV as part of their regular vaccine schedule. The study published in the Lancet this week concluded the HPV immunisation programme has successfully almost eliminated cervical cancer in women in the UK born since Sept 1, 1995. The study that was funded by Cancer Research UK comments that the findings were better than expected and that cervical cancer could become a rare disease. Vaccines save lives.